Origin/ Local – Referred pain – Trigger points – Muscle spasms – Phantom pain – Edema – Inflammation- Hernia prevention
Sexual intimacy is not discussed openly in a lot of societies. Men, Women, including Teenagers and Seniors can have problems:
- Inability to consummate relationship due to pain, miscues
- Erectile Dysfunction
- Timing Incoordination
- Muscle Spasms
- Pain prior to penetration
- Pain During and After penetration
- Scarring
- Inflammation
- Frequent Infections from intercourse
You can discuss these issues with us and we can help you work on one step at a time.
Also see link to a research recruitment that is being done in Canada:

Abdominal and Gastro-Intestinal Pain

The Digestive Tract is a long pipe made entirely of muscles and soft tissues. At each level there are different components of digestion taking place. The tract, made of smooth muscles, can contract/ relax to allow for normal motility and to facilitate the digestive process as food is moved down and converted to nutrition or to waste products. Any problems along the pipe is like "traffic jam", affecting normal flow and causing backed up, muscle spasms, reducing digestive function.
Imagine a processing factory with many unhappy or unhealthy workers. Disruption of flow at any stage will result in problems. Imagine Lucy and the Chocolate Factory!!! Or Charlie Chaplain! In these cases, there are clumsy or uncoordinated comedians lurching around. In real life, there can be blockages, adhesions, spastic muscle contractions (cramping), or pressure from bloating, etc. For someone having pain, this is no joke. We have to find out which sections are problematic and why, then help give you proper treatment.
The fascia protect and cushion the organs. Surgical procedures can form scar tissue and adhesions blocking flow. Myofascial and visceral manipulation can help improve normal muscle mobility and digestive motility, improve nerve and vascular flow, then in turn reduce pain.
On the outer layer, abdominal muscles are circumferentially wrapped around to protect the organs. They are voluntary muscles that contract/ relax along with the breathing diaphragm muscle on top, and pelvic floor muscles at the bottom.
Often, we forget that we can use these muscles to compress and to expand for better flow of digestion and breathing. We can also use these muscles coordinating with pelvic floor contractions to improve control of our core and pelvic floor.
Proper usage of abdominal, diaphragm and pelvic floor muscles will prevent wrong pressure build up, thus preventing prolapse or herniation, while further strengthening the trunk and core for daily functions.
History of injury, trauma, dietary changes, life stresses, age, and health status, lack of exercise, and many more factors can create imbalance and weakness, inflammation, muscle atrophy, herniation, etc.
Hernias, Hemorrhoids, and Prolapse Prevention:
- when a worker or athlete tries so hard to perform, such as pressing weight, doing crunches, lifting heavy objects, etc., many times you forget to breath, or you hold your breath, push down on your abdomen and pelvic floor, do maneuvers called "Valsalva".
You increase your risk of getting herniations, and or urinary or fecal leakage.- Each time you do it wrong, you are stressing the pelvic floor, groin, or abdomen the wrong way. Sooner or later, when you really need to perform at the top of your game, you may end up getting a hernia, or start leaking instead.
- You could have a prolapse or protrusion of the bladder, uterus(for females), large intestine, or rectum, into the pelvic floor or outside of the body
- Men would have painful inguinal or scrotal hernias
- Hemorrhoids also occur with a lot of pushing and straining activities, inflaming the linings and opening of the rectum.
- It's very important to learn from the outset how to stabilize your core muscles, get into good postural alignment, breath correctly. You must learn how to COORDINATE your breathing to move your body correctly.
- You need to know HOW to CORRECTLY recruit your pelvic floor to further support your activities.
Abdominal and Gastrointestinal related problems can cause pelvic floor inflammation and problems:
- IBS (Irritable Bowel Syndrome) causes prolonged and chronic irritations in the digestive system and into the voiding organs: the rectum and anus.
- Frequent diarrhea or constipations irritate not just the linings of the rectum but also the muscles of the intestines, rectum, and anal sphincters. Too much pushing or voiding causes chronic pain and irritations.
- We can start treatment to reverse or reduce some of those symptoms, prevent them from worsening into a global pelvic floor spasm
- IC (Interstitial Cystitis) in women also cause spasms and pain, inflammatory response in the abdominal and pelvic areas
- In men, Prostate enlargement or inflammation can cause spasms and or voiding issues.
- Prostate surgeries result in incontinence as well
Gastro-Intestinal problems, indigestion, chronic inflammation, bloating, frequent urination or bowel problems will place too much pressure onto the pelvic floor and genitals, which in turn can create pain and muscle spasm problems.
Pelvic Pain
- Pudendal nerve pain: Prolonged sitting on a small bike seat for prolonged bike riding may compress your pudendal nerve, causing pain in the pelvic floor and refer pain into the genitals.
- Prolonged flexion (bending) of your hips or back can compress blood flow into your abdominal area, causing organ dysfunctions, such as constipation, diarrhea, irritable bowels
- Back pain can lead to pelvic pain: the spinal nerves and muscles can be compressed, causing abnormal nerve interruptions, poor circulation to the pelvic floor and abdomen.
- Sacro-iliac pain and immobility: stresses or excessive movements, or tightness in the Sacro and Illiac junctions can cause pain and muscle spasms
- Lumbosacral injuries, Low back and Sacral or Coccyx pain or compression would cause localized and referred pain into the abdominals, pelvic floor, or even into your legs
- Falling directly on the tail bone (coccyx) can cause severe pain and immobility, muscle spasms locally and further into the deep muscles of the pelvic floor
- Hip/ groin pain could cause tightness and muscle spasms in the pelvic floor
- Prolonged running, squatting, climbing activities may over stretch your legs and inner thigh muscles, overworking your spinal muscles and spinal segments, sacral illiac joints, or over work your hip joints.
- The pubic symphysis can also be stress and over stretched causing pain.
- Proper bracing, strengthening, stabilization exercise will help to control and prevent these types of problems.
Some examples of problems with the FEMALE Pelvic Floor
This diagram below shows multiple factors causing increased pain and tension. These problems cause muscles spasms, irritation, and chronic pain. Repeated problems increases and worsen the pain cycle.
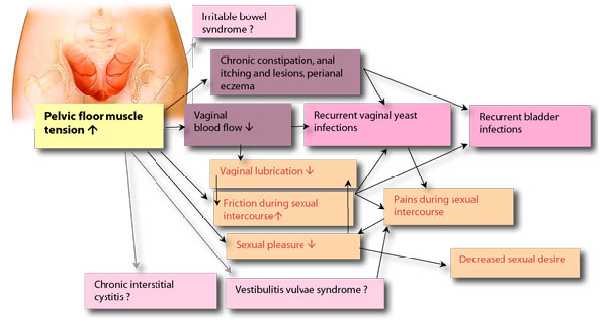
Women who had problems with abuse or violent partners often have multiple psychosocial problems, physical pain, depression, insecurities, all of which are intertwining in causation and results in chronic manifestation in pain, inflammation, weakness.
Men
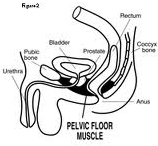 In men, many problems can be addressed with exercises and self help. Surgeries and voiding patterns, prostate health or any other surgical procedures might affect the male organs and pelvic floor.
In men, many problems can be addressed with exercises and self help. Surgeries and voiding patterns, prostate health or any other surgical procedures might affect the male organs and pelvic floor.
Treatment for men would involve approaches to the area between the penis and the rectum, or inside the rectum. Problems of erectile dysfunction, especially after surgical procedures, can improve with electrical muscle stimulation and biofeedback.
Prolapse
In both women and men, there are also issues of organ prolapse- the rectum can protrude outside of the anal cavity especially during pushing with voiding. In women, because of the vaginal space, the bladder or rectum can sink into the vaginal walls. In these cases, a pessary or sling, or surgery may be needed to contain the problem.
Abdominal and Spine Considerations
Many times, there might be pain in the pelvic floor without problems relating to continence. A person can have pain with the muscles and soft tissue inside or outside the pelvic floor. There are many causes of pelvic pain in women and men, including bladder infections, irritable bowels, pelvic inflammatory diseases, uterine fibroids, scar tissue adhesions, urinary tract infections, vulvodynia, dysparunia (pain with intercourse). Many problems will develop trigger points, referring pain out to the pelvic floor, low back, and abdomen.
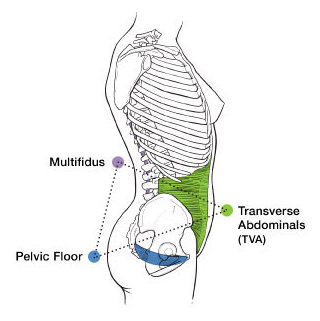
Pain
Pain in the low back and abdomen also refer to the pelvic floor. Any problems in the legs and feet may cause muscle guarding, pain reactions, holding patterns, postures that will affect pelvic floor functions. Any poor postures from the head, shoulders, spine, can result in abnormal holding of the pelvic and spine area. Therefore, when someone has problems, all aspects of a person must be considered. Pain treatment is determined by the source of the problem as well as treating local symptoms.
Physical Disability
Do not forget patients with an existing physical disability. Many are born with muscle tone spasticity or flaccidity. Some patients become disable later in life such as spinal cord or head injury, or stroke, etc. They have special continence, pain, voiding issues that might need more intervention and medications to help.
Summary of home programs:
- Start a log of voiding pattern, pain, what you are doing during this time
- Start a general exercise routine including movements of arms, legs, trunk, pelvis
- Focus more on pelvic floor exercises – ask a physical therapist pelvic floor specialist for correct techniques
- Massage belly and back, pelvic floor
- Use heating pads to help
- Find time during the day for quiet and relaxation (calming of tension) at least 5-10 minutes
- Work on deep diaphragmatic breathing with exhalation and relaxation
- Check your posture for good alignment
- Look into biofeedback or electrical stimulation if exercises do not help sufficiently
- Ask your doctors, including a good urologist, urogynecologist, gynecologist, and physical therapist who specialize in pelvic floor rehab and pain treatment.
In Summary,
If you experience pain, or see a trend of having pain and discomfort in the abdomen, pelvis, or hip areas, leaking of urine or fecal matters, inflammation or irritation of the genitals after daily activities, call us for consultation.
We determine if problems are musculoskeletal spasms, abnormal patterns of recruitment, and or movement related.
We provide treatment interventions (manual therapy, feedback, trigger point release, stretching, exercises, etc) and instruct appropriate body mechanics, home programs to help relieve pain and help you take better care of yourself.
Do NOT accept your problems as "Normal" or "Unfixable". If you can't get help from someone, go find help elsewhere- don't give up!
Pelvic Floor problems can take a long time to improve, but many can be resolved or at least become manageable.
We're looking forward to helping you feel better.
Make your appointment with us at 813-631-9700



